
![]()
![]()
![]()
![]()
Conception to Birth
Learning Objectives
- Recognize the association between periodontal disease and poor birth outcomes
- Describe the putative biologic pathway underlying this association
- Identify potential interventions and describe status of intervention trials
-
Describe current status of guidelines for oral health care of pregnant women
In This Section
You will follow Mrs. Perez through her third pregnancy, learn about her periodontal disease, and consider the relationship between her oral health and pregnancy
Table of Contents
The Parent: Mrs. Perez
Questions for Mrs. Perez and her Unborn Child
What is Periodontal Disease?
Periodontal Disease: Poor Birth Outcomes
Effectiveness and Evidence for Intervention
Dental Care for Pregnant Women
So What Happened in the Case of Mrs. Perez?
The Parent: Mrs. Perez
|
Introduction to Mrs. Perez: Her Oral Health Status and Pregnancy Experience |
Meet Mrs. Perez. She is a 32-year-old Hispanic mother of 2 children under the age of 6 years and pregnant with her third. She presents to the dental clinic at her local community health care center complaining of bleeding gums and a loose tooth. She reports no acute dental pain but describes generalized oral discomfort that intermittently makes eating difficult. Mrs. Perez has delayed seeking dental care because of long wait-times at the health center dental clinic, lack of funds to pay for care, lack of dental coverage as her state eliminated adult dental coverage in its Medicaid program, and difficulties finding care for her two young children.
At Mrs. Perez's dental examination, the dentist informs her that she has periodontal or gum disease. Her dentist explains that this disease is caused by a bacterial infection, is chronic and slowly-progressing, is typically painless until advanced, and is the reason for her bleeding gums and loose tooth.
How typical is Mrs. Perez?
* Oral health disparities: Hispanic and African Americans experience higher rates of oral disease and tooth loss than white, non-Hispanics (1)
* Dental insurance coverage: Half of all Americans have no dental insurance nearly three times more than have no medical coverage.
* Financial barriers to care: Nearly three-quarters (72%) of US adults not obtaining dental care in a year report that the major reason is financial (4)
* Dentists participation in Medicaid: Few dentists participate in Medicaid. Approximately 1/3 of all US dentists provide at least one dental service under Medicaid but only 14% are active Medicaid providers (defined as those who bill more than $10,000 in a year) (5)
* Dentist workforce trends: There are approximately 2 dentists graduating for every 3 nearing retirement leading to a decline in the ratio of dentists to population. Rural and inner city areas are experiencing declines faster than other areas. As of June 2003, nearly 9000 additional dentists would be required to achieve a targeted 1:3,000 dentist-to-population ratio in designated dental shortage areas. (6)
* The color of dentistry: The number of underrepresented minorities in the dental profession is significantly lower than their proportion in the overall population (5.7% of graduate dentists are African American and 5.3% are Hispanic while 12% of the US population is African American and 11% is Hispanic) (7).
* The dental safety net: The dental safety-net, comprised of dental schools, community health centers, dental clinics and mobile van programs, are few in number compared to the medical safety net, primarily because community hospital emergency rooms rarely provide dental care beyond palliative services. (54)
* Adult dental Medicaid coverage: Nationally only about 1% of Medicaid expenditures go to dental care (8) and fiscal pressures have led to reductions and eliminations of dental benefits for adults and the disabled. In 2005, only 8 States had reasonably comprehensive adult dental coverage under Medicaid. (53) (In contrast to adult coverage, Medicaid's EPSDT benefit mandates comprehensive dental coverage for covered children from birth to age 21.)
|
Questions for Mrs. Perez and her Unborn Child
What happens if Mrs. Perez does not receive the necessary dental treatment for her periodontal disease? The most obvious consequence will be continued mouth pain, disease progression and eventual tooth loss. But what about the systemic effects of her periodontal disease? How will her oral disease affect her pregnancy or her unborn child?
What is Periodontal Disease?
American Academy of Periodontology web information on periodontal disease
NIH web information on periodontal disease
Periodontal disease is a chronic infectious disease caused by various gram negative bacteria existing below the gum line in the form of soft plaque that colonizes tooth surfaces and associated hard calculus (tarter) that adds a physical irritation. Periodontal disease causes inflammation and associated bleeding gums and progresses to destruction of the bone that supports teeth. As the tooth support gradually weakens, teeth become mobile and are eventually lost. Individual response to this infection varies widely so that some people are more susceptible to this consequences of this disease.
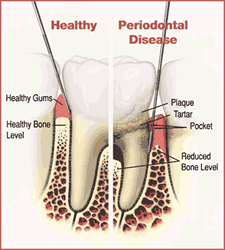
Source: AAP
Periodontal (Gum) Diseases
For more on periodontal disease, NIH has a free publication available at: http://www.nohic.nidcr.nih.gov/health/nohic_forms/orderpubs.asp
Periodontal Disease: Poor Birth Outcomes
March of Dimes web information on Low Birth Weight
Preterm Low Birth-weight (PLBW) pregnancy outcomes in the U.S. remain a concern because of the significant consequences to maternal and child health, high costs, long-term disease burden, and individual suffering. The economic consequences exceed $5 billion annually. PLBW pregnancy outcomes account for 6-9 percent of all births (9)
The Centers for Disease Control and Prevention reports that the second leading cause of infant mortality is low birth-weight associated with prematurity (10). PLBW accounts for 70% of all perinatal deaths and 50% of long-term neurologic morbidity (9).
Known causes of PLBW, that may be medically managed and include: asthma, cigarette smoking, bacterial vaginosis and diabetes. However, much of its incidence remains unexplained and periodontal disease may explain a substantial proportion of this mystery. NIH reports that as many as 18% of the 250,000 premature low-weight infants born in the United States each year may be attributed to infectious oral disease (11). The classic measures for association between exposure (periodontal disease) and outcome (PLBW) are being explored and suggest possible causality. Based on this emerging science, there is hope that the severe developmental, behavioral, health, and economic consequences of PLBW may be minimized by improving oral health during pregnancy.
State of the Science |
Human Observational Studies:
Human Interventional Studies:
|
Effectiveness and Evidence for Intervention
Can treating periodontal disease in pregnancy reduce poor birth outcomes?
Two studies have shown an association between treating periodontal disease during pregnancy and improved birth outcomes (16, 17).
For the mother, there are no known negative consequences associated with improving the oral health of pregnant women. The potential positive outcome may be reduced poor birth outcomes. Thus, there is growing enthusiasm for promoting optimal oral health and dental care during pregnancy.
Dental Care for Pregnant Women
The National Healthy Mothers, Healthy Babies Coalition (HMHB), issued a position statement asserting that oral health care during pregnancy is crucial and should be available to all women, regardless of income level. HMHB is committed to working with dental and other health care providers to increase awareness of, and support research on, the possible link between periodontal disease and pre-term, low birth-weight babies (18)
The American Academy of Periodontology has developed a draft policy statement that recommends pregnant women have a periodontal examination performed and appropriate preventive and/or therapeutic services provided, as there is emerging evidence that women with periodontal disease may be more at risk to deliver a preterm low birth weight baby. Consumer and media information are posted on the web at: http://www.perio.org/consumer/pregnancy.htm
Clinical guidelines suggest that routine plaque and calculus removal via polishing, scaling and curettage can be performed safely during pregnancy, regardless of trimester (19) but the most conservative approach saves dental treatment for the second and early third trimester. Dentists and obstetricians agree that routine dental care should be maintained throughout pregnancy(20,21). However, despite the growing evidence and literature to support the association between periodontal disease and PLBW, this recommendation has not been widely translated into clinical or public policies and pregnant women and their obstetricians have noted that many dentists are hesitant about caring for pregnant women.
|
Medicaid Dental Coverage for Children, Mothers, and Pregnant Women |
Medicaid programs, administered by the states within federal guidelines, are required to provide certain populations with specified (mandatory) benefits. Dental is only mandated under Early and Periodic, Screening, Diagnostic, and Treatment Services Program ( EPSDT) and is therefore available to pregnant adolescents but not typically to pregnant women over 21. Pregnant women over age 21 who are in Medicaid therefore can only access dental benefits in states that elect to provide it (22). As the federal and state governments seek Medicaid cuts, elective dental services have been susceptible to termination. As of 2005, only 6 states provided reasonably comprehensive dental benefits to adults while others provide emergency treatment or no dental benefit at all. For information on erosion of dental Medicaid coverage for adults click on Children's Dental Health Project brief, Preserving the Financial Safety Net by Protecting Medicaid and SCHIP Dental Benefits
California: first in the nation to extend dental benefits to pregnant women |
|
The addition of preventive periodontal treatment to the scope of California Medicaid benefits for women in the pregnancy services only and pregnancy and emergency services only aid categories is estimated to potentially save over $24 Million annually by reducing PLBW by 2655 cases based on an anticipated 50% program effectiveness (23).
So What Happened in the Case of Mrs. Perez?
Mrs. Perez was unable to undergo periodontal treatment as she could not afford to pay for the service out-of-pocket and was not in a state that provided adult dental Medicaid coverage. Six months after her visit to the health center dental clinic, she delivered a preterm low birth-weight baby girl, named Maria. Fortunately, with advances in neonatal care, survival rates of pre-term low-birth-weight babies have dramatically improved. Unfortunately, studies indicate that pre-term children suffer from a multitude of acute and long-term problems, including significant delays in physical and psychological growth and development of all structures, including the craniofacial complex and teeth. Oral structures, like other tissues, are affected by prematurity and low birth-weight (24)
To learn more about Maria and her oral health, click on the navigation links at left or on the Early Childhood Caries pictures below.
 |
 |
 |
 |
